Dialysis Toolkit
Toolkit to support implementation of the ISN framework for developing dialysis in low-resource settings
Welcome to this toolkit. In 2021, in recognition of the growing need for kidney failure treatment in low resource settings, the ISN published a framework providing guidance to policy makers and healthcare providers wishing to develop dialysis programs.
Endorsed by the WHO, this technical package drew attention to several key elements, including affordability, sustainability, scalability and equity. The purpose of this toolkit is to provide materials that support the ISN framework through educational videos, webinars and links to online resources. They are primarily intended for policy makers and healthcare providers but will undoubtedly be of use to people in need of kidney replacement who wish to be better informed about treatment options and how services can be structured. The patient voice is key for service development, and we hope that this toolkit will empower people with kidney failure, their families and carers, to advocate for improved services.
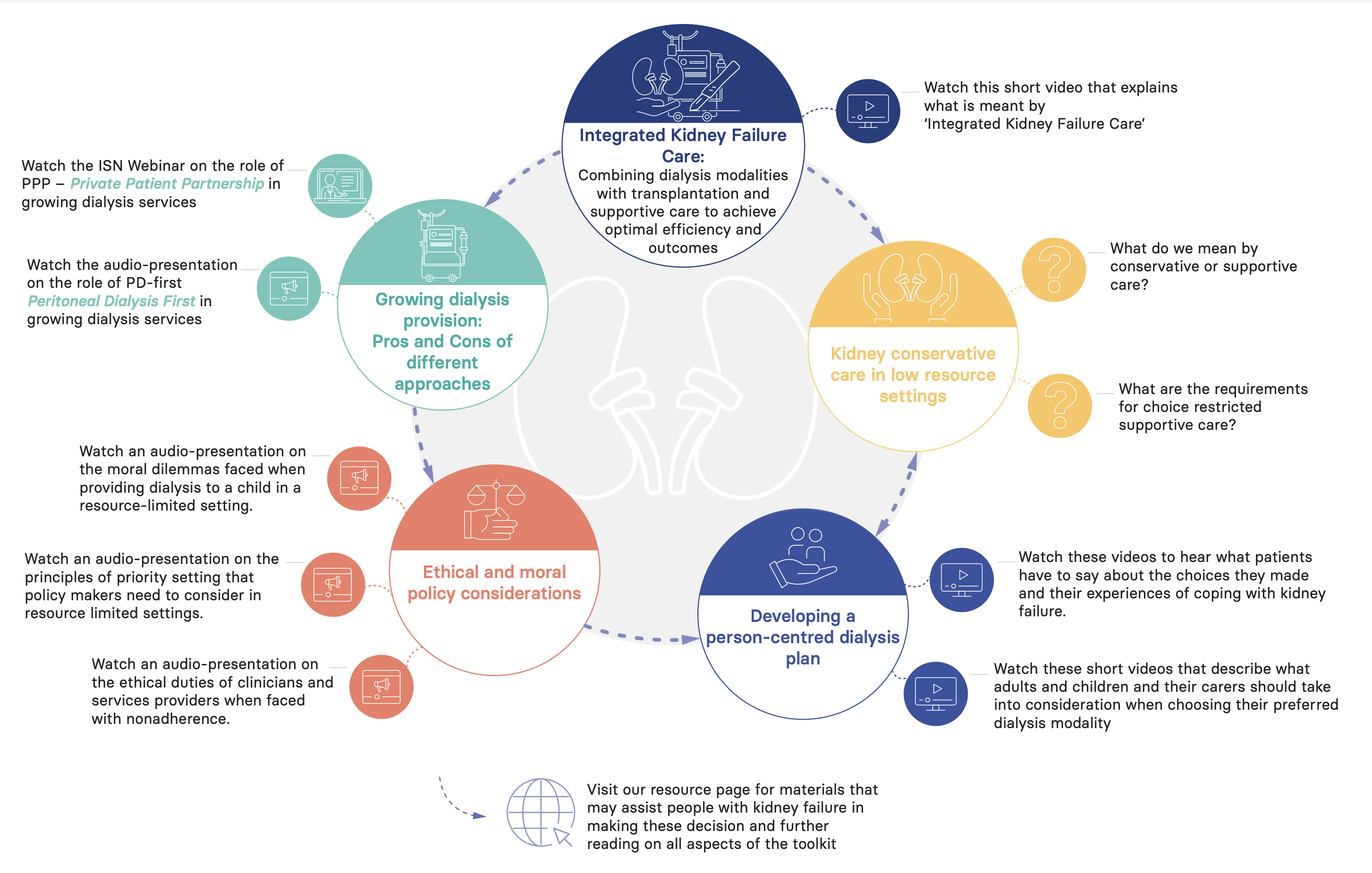
The components of the toolkit are shown here in overview, organised according to the key components of the framework. Starting with an explanation of what is meant by integrated kidney care, it covers approaches to growing dialysis provision that have proved useful in low resource settings, proceeds to guidance on the ethical and moral concerns that should be considered and finally focusses on the individual with the development of a person-centred dialysis plan. It does not cover the requirements for delivery of dialysis, including quality, standards and resources, topics that will be covered elsewhere in the ISN Kidney Failure (KF) Strategy. Equally the section on conservative or supportive care, an essential component of any kidney failure service, links to ISN KF strategy which is still in the process of development.
This toolkit was developed by: Simon Davies, Niang Abdou, Brett Cullis, Ana Elizabeth P L Figueiredo, Arpana Iyengar, Valerie Luyckx, Henriette Nygård, Jordan Parsons, Irma Tchokhonelidze, Isaac Teitelbaum and Tushar Vachharajani
Integrated Kidney Failure Care: Combining dialysis modalities with transplantation and supportive care to achieve optimal efficiency and outcomes
Watch this short video that explains what is meant by ‘integrated kidney failure care’
Watch the ISN webinar on the role of Private Patient Partnership (PPP) in growing dialysis services.
Growing dialysis services in any setting can be a challenge but especially so when resources are limited. One way of achieving the capital investment required to develop dialysis services is through public private partnership (PPP). This webinar is focused on what such partnerships can achieve, providing participants with an in depth understanding of both the benefits and the potential disadvantages and how to mitigate against these. Starting with a description of a successful PPP implementation from Georgia, the panel shares experiences from around the world and attempt to define PPP, recognizing that this definition will differ by jurisdiction. Key aspects of the discussion includes standards, costs, contracts, scope of the service (what should, must or must not be included), ethics, management of uncontrolled growth and third-party costs (e.g. out of pocket expenses).
Watch the presentation on the role of Peritoneal Dialysis First (PD-first) in growing dialysis services.

Introducing a national policy by which all new people with kidney failure start their treatment with peritoneal dialysis, “PD-first”, has proved an effective way of introducing a universal healthcare programme for renal replacement. This approach was first adopted in Hong Kong and remains highly effective and is associated with excellent outcomes. It requires effective government negotiation for competitive pricing of dialysis fluids and reduces the infrastructure costs associated with building and staffing haemodialysis units. It does however lead to a restriction in choice and over time there will be the need to invest in haemodialysis services.
Watch this video on the moral dilemmas faced when providing dialysis to a child in a resource-limited setting.
As clinicians navigate through pathways of kidney failure care, from conservative management to dialysis and transplantation, one is faced with a combination of medical, social and ethical issues. Addressing such issues demands a sound understanding of the principles of bioethics by the clinician to maintain the right conduct and standard of behaviour. In this presentation, using real life examples we discuss key ethical challenges in the care of adults and children with kidney failure. In the context of under-resourced settings where lack of accessible dialysis therapies and insufficient resources prevail, ethical dilemmas can lead to moral distress. There is a need to increase awareness of ethical issues, understand its implications and provide strategies for shared decision making in the management of patients with kidney failure.
Watch this video on the ethical duties of clinicians and service providers when faced with nonadherence.
This video explores some of the key ethical considerations when a patient does not adhere to an agreed treatment plan. Highlighting various examples of nonadherence, it examines and applies important ethical principles. These range from respect for patient autonomy and justice to proportionality and respect for dignity. Finally, it provides practical advice on navigating such situations whilst upholding professional ethical duties.
Watch this video on the principles of priority setting that policy makers need to consider in resource-limited settings.
When budgets are constrained, governments have the obligation to set priorities for health and determine which services will be provided under universal health coverage and which will be “left out”, meaning the patient will have to pay out of pocket. This talk discusses the process of priority setting around provision of care for kidney failure, focusing not only on cost-effectiveness, but also on the importance of considering equity in the priority setting process, to promote fairness in resource allocation. It is unlikely that universal health coverage can be extended soon to cover the needs of all patients with kidney failure in lower resource settings, but the commitment to progressive expansion of coverage over time is important, and must begin with transparency and accountability in the priority setting process today.
Watch these short videos that describe what adults and children and their caregivers should take into consideration when choosing their preferred dialysis modality.
Watch this video to hear what patients have to say about the choices they made their experiences of coping with kidney failure.
Developing a person-centred dialysis plan – resources for patients, their relatives, carers and their healthcare professionals
There are a number of non-commercial online resources designed for patients to help them understand more about kidney failure and the treatment options available. In general these are not primarily aimed at people living in low/low-middle income countries so patients from these countries should be made aware that the choices discussed, which may include variations on the main modality – such as home haemodialysis or automated peritoneal dialysis may not be available. Despite this the group developing the toolkit found them valuable and educational. Remember, when using YouTube it is possible to change the language of the subtitles https://youtu.be/ZnoxutAvyaI?si=_XOLDVjnq16Sj58z
Failing Kidneys and Different Treatment Options
This Canadian Video by Mike Evans starts with an excellent summary of the functions of the kidney and what can go wrong in kidney failure – and how to recognise the symptoms. It discusses the options for treatment including transplantation (0.52 mins), conservative care (2.10 mins), getting a kidney from a living donor (3.11 mins), haemodialysis (4.05 mins) and peritoneal dialysis (4.50 mins).
The UK National Kidney Federation Website presents unbiased information pages about:
Peritoneal Dialysis
Haemodialysis
This video gives information for patients about the diet in kidney failure and advice about dietary restriction, which comes in several languages.
- Link to the English versionhttps://youtu.be/pELs1GfjmQU
- Link to other languages: https://m.youtube.com/playlist?list=PLxIt6TW5JJ8EveshkmHspD9RJCELuU08Z ]
- Link to webinar addressing shared decision-making for dialysis in low-resource countries
Supporting shared decision making
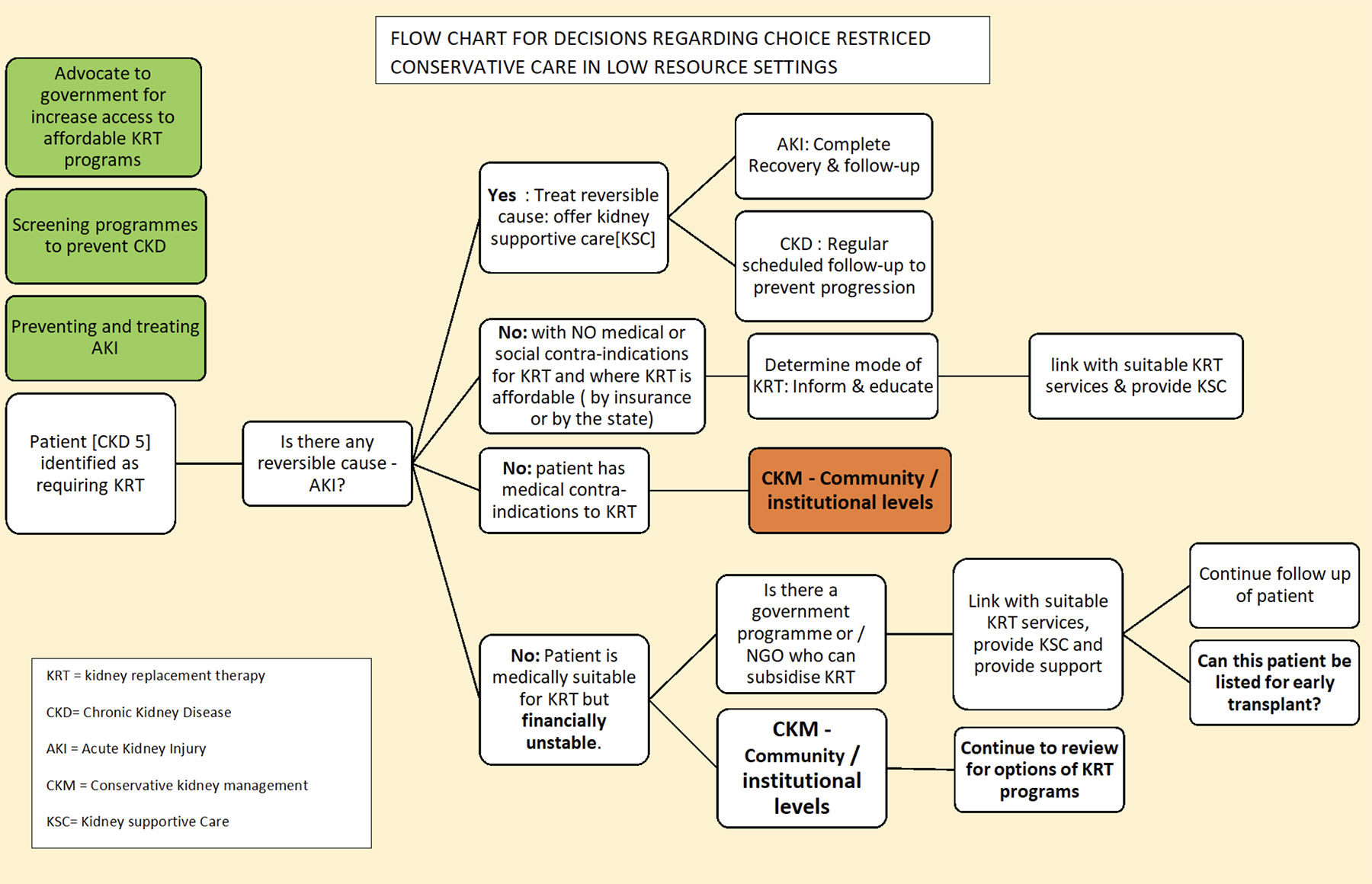
Unfortunately options for dialysis and/or different dialysis options in LMICs may well be restricted. Even under these circumstances there are likely to be decisions to be made – even if it is between having dialysis versus ‘choice restricted’ conservative or ‘supportive’ non-dialytic care (for these definitions see section on Conservative Care). All these decisions should be made in the context of shared decision making and to support this there are decision aids available to help structure this process and give unbiased advice. One such decision aid is available from Kidney Research UK which also includes links to multiple resources for patients and explanations about the functions of the kidney and kidney failure. It is endorsed by the UK National Institute for Health and Care Excellence (NICE), European Best Practice Group, and Quality tested by the International Decision Aid Library Inventory System.
https://kidneyresearchuk.org/wp-content/uploads/2019/05/KR-decision-Aid-DOWNLOAD.pdf
Resources to accompany the Videos in the Toolkit and additional information.
The ISN framework for developing dialysis programs in low-resource settings.
https://www.theisn.org/wp-content/uploads/2021/03/ISN-Framework-Dialysis-Report-HIRES.pdf
PD first Policy
- Peritoneal dialysis first policy in Hong Kong for 35 years: Global impact. Li, P. K-T. et al, Nephrology. 2022;27:787–794. https://doi.org/10.1111/nep.14042
- A global overview of the impact of peritoneal dialysis first or favored policies: an opinion Liu, F.X. et al, Peritoneal Dialysis International, 35, pp. 406–420 https://doi.org/10.3747/pdi.2013.00204
- Economic Evaluation of Palliative Management versus Peritoneal Dialysis and Hemodialysis for End-Stage Renal Disease: Evidence for Coverage Decisions in Thailand; Teerawattananon, Y et al. Value in Heath, 2007;10:61-71 https://doi.org/10.1111/j.1524-4733.2006.00145.x.
- Economic evaluation of peritoneal dialysis and hemodialysis in Thai population with End‑stage Kidney Disease. Assanatham et al. BMC Health Services Research (2022) 22:1384 https://doi.org/10.1186/s12913-022-08827-0
- Peritoneal dialysis–first initiative in India: a cost-effectiveness analysis Clinical Kidney Journal, 2022;15:128-135 https://doi.org/1093/ckj/sfab126
- Lifetime cost-effectiveness analysis of first-line dialysis modalities for patients with end-stage renal disease under peritoneal dialysis first policy. Wong et al. BMC Nephrology (2020) 21:42 https://doi.org/10.1186/s12882-020-1708-0
Private Public Partnership
- The Georgia Model. Tchokhonelidze I. Global Dialysis Perspective: Georgia. Kidney360. 2023 Jan 1;4(1):106-109https://pubmed.ncbi.nlm.nih.gov/36700912/
Ethical Considerations
- Priority Setting as an Ethical Imperative in Managing Global Dialysis Access and Improving Kidney Care https://www.sciencedirect.com/science/article/pii/S0270929521000747
- Making Fair Choices on the Path to Universal Health Coverage https://apps.who.int/iris/handle/10665/112671
- Three Case Studies in Making Fair Choices on the Path to Universal Health Coverage https://www.hhrjournal.org/2016/11/three-case-studies-in-making-fair-choices-on-the-path-to-universal-health-coverage/
- Health technology Assessment (WHO): https://www.who.int/health-topics/health-technology-assessment#tab=tab_1
- Why have Non-communicable Diseases been Left Behind? https://link.springer.com/article/10.1007/s41649-020-00112-8
- Guidance on priority setting in health care (GPS-Health): the inclusion of equity criteria not captured by cost-effectiveness analysis https://resource-allocation.biomedcentral.com/articles/10.1186/1478-7547-12-18
- Extended cost-effectiveness analysis: https://www.hsph.harvard.edu/stephane-verguet/extended-cost-effectiveness-analysis-ecea/
- Fair Allocation of Scarce Medical Resources in the Time of Covid-19. https://www.nejm.org/doi/pdf/10.1056/NEJMsb2005114?articleTools=true
- Setting Limits Fairly: https://www.amazon.com/Setting-Limits-Fairly-Learning-Resources/dp/0195325958
- UHC Indonesia: https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(18)31647-7/fulltext
- Parsons JA, Taylor DM, Caskey FJ, Ives J. 2021. Ethical duties of nephrologists: when patients are nonadherent to treatment. Seminars in Nephrology 41:262-271.
https://doi.org/10.1016/j.semnephrol.2021.05.007
- Key ethical challenges in providing dialysis in low–resource settings — A view from the trenches: https://pubmed.ncbi.nlm.nih.gov/36694392/
- Addressing the Ethical Challenges of Providing Kidney Failure Care for Children: A Global Stance: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8963107/
- Considering Family Resources When Making Medical Recommendations: https://pubmed.ncbi.nlm.nih.gov/29196504/
Guidance for Primary Care: Kidney Replacement Therapies and Conservative Kidney Management
 Access the resource here.
Access the resource here.
The toolkit was developed by the ISN Dialysis Toolkit Working Group
Simon Davies | Keele University, UK
Tushar Vachharajani | Wayne State University, United States
Isaac Teitelbaum | University of Colorado, United States
Arpana Iyengar | St Johns Medical College Hospital,India
Brett Cullis | Mediclinic Hospital, South Africa
Valerie Luyckx | University Of Zurich, Switzerland
Ana Elizabeth Figueiredo | Pontifícia Universidade Católica do Rio Grande do Sul (PUCRS), Brazil
Henriette Tyse Nygård | Haukeland University Hospital – Norway, Norway
Abdou Niang | Dalal jamm hospital, Dakar, Senegal
Irma Tchokhonelidze | Nephrology Development Clinical Center, Tbilisi, Georgia
Jordan Parsons | University of Birmingham, United Kingdom