A continuous legacy of improving kidney health globally
Since 1960, the ISN has supported kidney care professionals and organizations around the world, empowering them to deliver better care and create lasting change in their communities. Our progress is made possible by the collective dedication of ISN members and partner organizations who generously contribute their time and expertise.
A snapshot of the difference made (2013-2023)
Trained healthcare professionals
Hospitals and clinics supported
Clinical projects funded
Members enabled to contribute expertise and time
Members who have benefitted from mentoring and leadership skills development
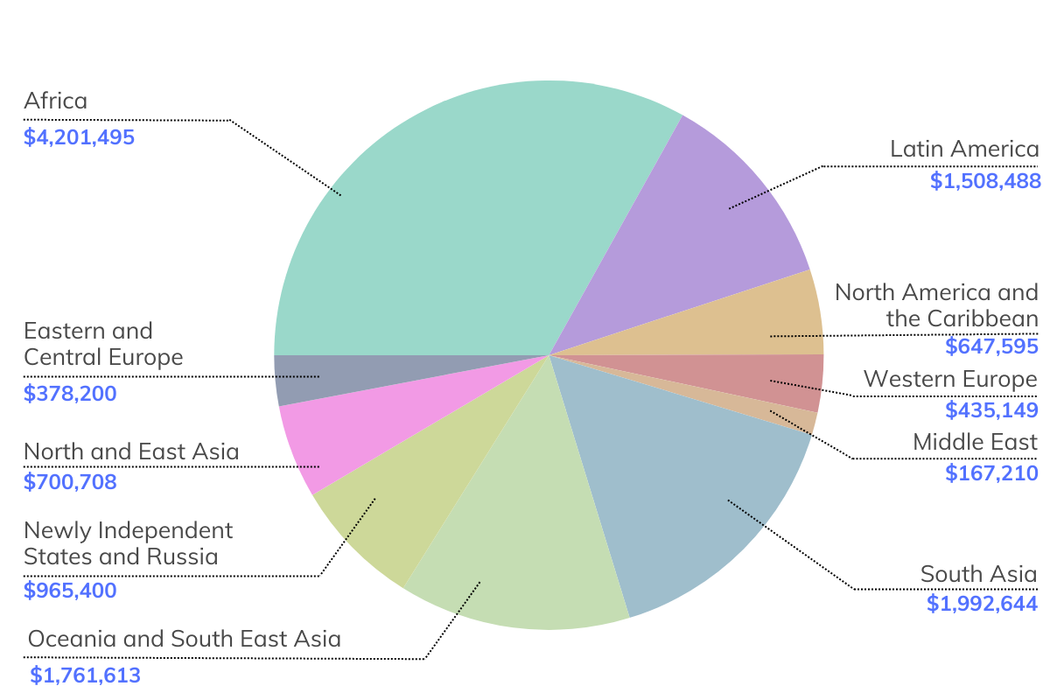
See the impact from 2013-2023
Explore the data on the interactive map to discover how the ISN’s work is empowering professionals, strengthening centers, and improving outcomes for patients across the globe. Click on a region or country to see how far we’ve come together.
* Click on the regions to see details
Hear from those the ISN supported
Behind every number is a story of growth and resilience. Meet those who either support or have benefitted from grants and initiatives, improving kidney care and making a difference where it matters most.
ISN Partner Organizations
The ISN works hand-in-hand with several partner organizations, encouraging intra-regional collaborations and enhancing training and education possibilities in selected fields of nephrology.












We would like to acknowledge the following partners that are currently supporting the ISN programs through unrestricted educational grants.




Transform kidney care with ISN Grants
Learn how our grants can help you grow your expertise, strengthen your organization, and contribute to a global effort to advance kidney health.