Caring for kidney patients in Malawi
In July 2014, a new hemodialysis unit opened in Blantyre, Malawi. Blantyre is in southern Malawi, not far from the border with Mozambique. With a population of over 600,000 it is the country’s second biggest city behind the capital Lilongwe, and is a major financial centre. Queen Elizabeth Central Hospital (QECH) is a tertiary referral centre for the entire Southern region in Malawi with over 1000 inpatient beds. There are around 30 medical admissions per day with over 200 general medical inpatients. The burden of kidney disease in both medical and non-medical patients is large.
I moved to QECH at the start of September 2014 and, already, the experience of working here has been beyond what I could have imagined from both a professional and personal point of view. The renal service here has been established and developed through the hard work of my colleague, Dr. Gavin Dreyer, who lived and worked here from 2011-14. We currently provide an inpatient renal referral service hospital-wide, we run a weekly renal outpatient clinic (adult), a monthly pediatric outpatient clinic, and provide renal replacement in those with both Acute Kidney Injury (AKI) and End Stage Renal Disease (ESRD). In addition to clinical work we have plans for a comprehensive study of AKI early next year.
Facilitated by Gavin, a contract was signed between the Malawi government and Fresenius in early 2014 to install five new hemodialysis machines at QECH. The unit was opened in July and all machines are fully functional without any major technical problems to date. The aim of our unit is to provide renal replacement to all patients with AKI requiring hemodialysis, and in a subset of patients with ESRD that are suitable for future transplantation. Transplantation is not currently possible here but it is our ultimate aim.
We hope to outline in detail the progress of our unit at the World Congress of Nephrology in Cape Town in 2015. In short, we have dialysed seven patients with AKI: four have recovered renal function; hemodialysis is ongoing in two, and one patient has died. We also have a current cohort of 19 chronic patients, six of whom have started hemodialysis within the last three months. Below are the stories of two of the patients we have recently treated with AKI.
Nicholas, age 24
Nicholas is a 24-year-old taxi driver who was involved in a road traffic accident in august. His taxi was hit by a lorry and he sustained multiple injuries. These included multiple rib fractures, a fractured pelvis and leg. He was treated on the Intensive Care Unit (ICU) at QECH where he developed oligoanuric AKI in the setting of hypotension/haemorrhage and presumed rhabdomyolysis (there is no capability to do creatine kinase here). Intubated and ventilated, we performed hemodialysis on our unit three times with subsequent complete recovery of renal function. He was discharged to home after a three-week inpatient stay.
I saw him in the renal outpatient clinic last week where I asked him about his experience in hospital and of the accident itself. He states he vaguely remembers being hit by the lorry but that the next thing he can remember is waking up in the ICU with his parents by his side. He didn’t know where he was but didn’t feel scared. He says he can’t remember coming for hemodialysis (sedated at this time). He is thankful, however, to the staff at the unit for their part in his overall recovery. Below are pictures of Nicholas when he came back to the unit after clinic last week to thank the nursing staff.
He is undergoing ongoing rehabilitation and his mobility is improving. He plans to go back to work as a driver early next year!
Arinafe, age 12
Arinafe lives in a village near Mulanje, which is a two hour drive south of Blantyre. She was previously well but became unwell around two weeks ago with a febrile illness, bloody diarrhoea, and abdominal pains. She was seen in the local hospital but transferred to QECH due to an acute liver injury and oligoanuric AKI. On arrival she was very unwell with marked jaundice (bilirubin 24mg/dL), bleeding (epistaxis and GI blood loss) presumed to be a consequence of her liver injury, subsequent anaemia, and AKI (creatinine 8mg/dL and potassium 6.7mmol/L).
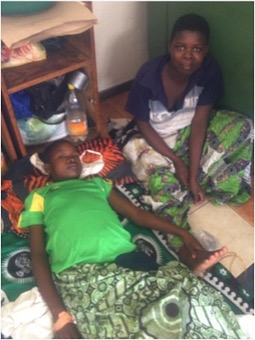
In pediatrics, we tend to favour acute peritoneal dialysis but due to her GI symptoms it was decided preferable to perform hemodialysis for solute control. A temporary femoral catheter was inserted and she has undergone four sessions of hemodialysis to date. Her liver injury is improving, as is her AKI, with urine output increased to 0.7ml/kg/day yesterday. Below is Arinafe with her mum recovering on the pediatric ward.
The cause of Arinafe’s AKI is unclear. Hepatitis B and C serology is negative, she has had normal platelets throughout and there is no history of known toxin exposure. Renal USS is normal. She has been treated with broad-spectrum antibiotics (to cover possible infection with Salmonella typhii and other gram negatives) and doxycycline (to cover possible Leptospirosis). We hope her renal function will continue to improve and we will be able to withdraw hemodialysis soon.