A Day in the Life of a Resident on a Nephrology Ward in Mexico
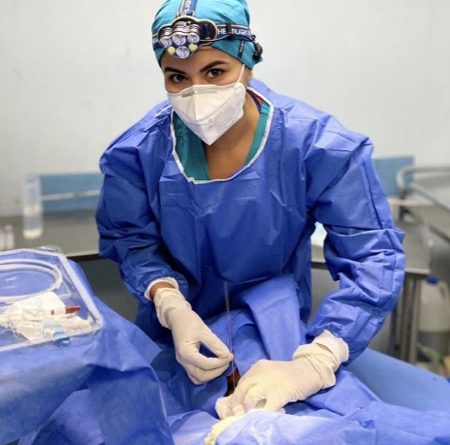
Alexia Romero placing a tunneled catheter for hemodialysis during one of her shifts at the Hospital Civil of Guadalajara
By Alexia Romero
My name is Alexia Romero, and I am a nephrology resident at the Hospital Civil of Guadalajara, a 1,200-bed tertiary care center in Mexico.
At the start of a new day in the nephrology ward, alongside two resident fellows and two undergraduate interns, I know it’s going to be a busy day.
I am responsible for approximately sixty patients with chronic kidney disease. My first activity of the day is to assess each patient on the ward. We review laboratory and imaging tests and discuss and modify treatment accordingly, focusing on vital signs, urine output, and fluid balance.
Later, I review the list of procedures that I will perform during the shift. I’ll need to place 2-3 ultrasound-guided catheters for temporary and permanent hemodialysis patients per shift. We will also have to do the procedures of percutaneous peritoneal dialysis catheters (1 -2 per shift), in addition to paracentesis and thoracentesis.
We’re in charge of the hospital’s two-floor hemodialysis unit, with 24 machines working five shifts a day. The work in this unit is very demanding, requiring a lot of time and energy. As a resident, I visit each patient, make recommendations, and take care of any issues that come up during the session. Sometimes urgent situations arise which need to be resolved immediately.
Other specialties often require our services to evaluate cases that could be kidney-related or involve electrolytes or acid-balance disturbances. These patients may develop acute kidney injury, but some of our interventions can improve the clinical evolution of the case and avoid the necessity of kidney replacement therapy (KRT). Sometimes, of course, this is unavoidable, and we initiate urgent KRT.
Another responsibility, perhaps the most demanding, is working in the emergency room, where we carry out an initial examination, administer urgent treatment and decide which patients require hospitalization. Finally, at the end of the shift (24 hours later), we meet up in the residents’ office, where new cases are presented to all residents and attending nephrologist in preparation for the following shift.
Despite my hectic schedule, I’m pleased to be learning so much. Thanks to the Young Nephrologists Committee sharing stories of young ISN members from different parts of the world, I know that many share similar experiences and we can create networks to support each other through our respective residencies.