Sept 2022 Edition


Impact Factor 2021
This eDigest presents recent publications in Kidney International Reports on the pathophysiology, progression, treatment, and validation of complement-mediated kidney diseases.
This eDigest highlights four original papers, in the field of complement-mediated kidney diseases, that have been published in Kidney International within the past few months.
KIDNEY INTERNATIONAL REPORTS ARTICLE |
 Dysregulation of the complement alternative pathway (AP) underlies the pathogenesis of C3 glomerulopathy (C3G), one of the worst prognosis primary glomerular diseases with high recurrence after kidney transplant. Unfortunately, there are no approved therapeutic agents for C3G.
Dysregulation of the complement alternative pathway (AP) underlies the pathogenesis of C3 glomerulopathy (C3G), one of the worst prognosis primary glomerular diseases with high recurrence after kidney transplant. Unfortunately, there are no approved therapeutic agents for C3G.
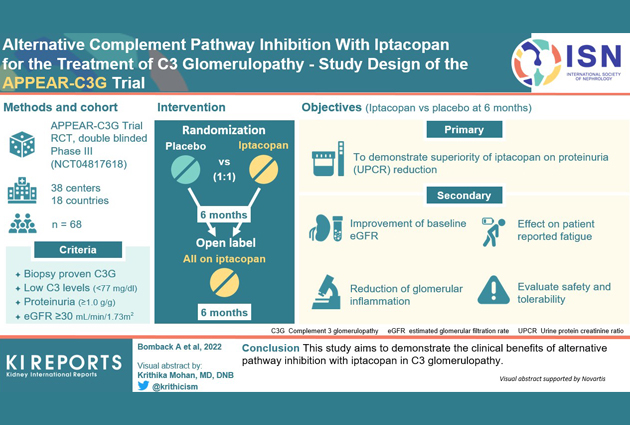
Iptacopan is a selective inhibitor of factor B, a key component of the AP. In a Phase II study, treatment with iptacopan showed a reduction in proteinuria and increased estimated glomerular filtration rate (eGFR) in patients with C3G.
APPEAR-C3G is a randomized, double-blind, and placebo-controlled Phase III trial that aims to evaluate the clinical efficacy and safety of iptacopan compared to placebo in patients with C3G.
Patients are randomized 1:1 to receive 200mg iptacopan twice daily or placebo for six months, followed by open-label treatment with iptacopan twice daily for all patients for six months.
Could iptacopan help improve kidney outcomes in C3G patients? Is it safe to use? Bomback et al. will soon have the data to answer these questions.
 In this paper, Bagchi et al. attempt to externally validate the international IgA nephropathy prediction tool in an Indian cohort believed to have a higher risk of rapid deterioration of kidney function. Their single-center retrospective study cohort included 316 patients with a median follow-up of 2.8 years. The primary outcome was a 50% reduction in GFR or renal failure, met in 87 patients.
In this paper, Bagchi et al. attempt to externally validate the international IgA nephropathy prediction tool in an Indian cohort believed to have a higher risk of rapid deterioration of kidney function. Their single-center retrospective study cohort included 316 patients with a median follow-up of 2.8 years. The primary outcome was a 50% reduction in GFR or renal failure, met in 87 patients.
To calculate the linear predictor and prediction probability of the primary outcome for each patient, they used models with and without race proposed by the original study. The variables in the model were age, eGFR, mean arterial pressure, proteinuria, prior use of renin-angiotensin-aldosterone system blockers, immunosuppression at the time of kidney biopsy, and MEST score. In the model with race, patients were classified as “other.”
Both the full models showed good discrimination concerning risk stratification in the South Asian cohort. Compared with the full model without race, the full model with race showed limited improvement in risk reclassification for predicting five-year risk. Both models underestimated the rate of progression compared with what was observed. The authors suggest that larger and more prolonged multi-center studies among South Asians are necessary before the IIgAAN prediction tool is adopted in clinical practice.
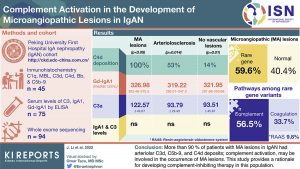
IgA nephropathy (IgAN) remains the commonest glomerulopathy worldwide, with a third of patients progressing to end-stage kidney failure. For patients with IgAN, arteriolar microangiopathic (MA) lesions are an independent risk factor for predicting prognosis. The underlying mechanism that leads to MA is poorly understood. In this paper by Li et al. (China), biopsies from 94 patients were assessed prospectively.
Biopsies from patients with IgAN who had MA lesions had more complement deposition, especially C4d, on renal arterioles compared to those with arteriolosclerosis and those without vascular lesions. In addition, these patients also had higher levels of Gd-IgA1 and C3a. Fifty percent of those with MA lesions had rare genetic variations in complement-related genes. These findings strongly suggest complement involvement in the development of MA lesions in IgAN and poor outcomes in this group of patients. This opens the possibility of using complement-inhibiting therapy for this condition.
Glomerular C4d Immunoperoxidase in Chronic Antibody-mediated Rejection and Transplant Glomerulopathy
 The absence of C4d in peritubular capillaries (C4dptc) frequently complicates the diagnosis of late antibody-mediated rejection (AMR), which is referred to as “C4d-negative” AMR. The authors hypothesized that capillary C4d (C4dglom) represents endothelial interaction with antibodies and could improve immunologic classification of transplant glomerulopathy (TG).
The absence of C4d in peritubular capillaries (C4dptc) frequently complicates the diagnosis of late antibody-mediated rejection (AMR), which is referred to as “C4d-negative” AMR. The authors hypothesized that capillary C4d (C4dglom) represents endothelial interaction with antibodies and could improve immunologic classification of transplant glomerulopathy (TG).
This retrospective study used immunoperoxidase to evaluate C4d in 3,524 consecutive kidney transplant biopsies from a single center. C4dglom was found in 16.5% of biopsies and C4dptc in 9.9%. C4dglom was found in 60.3% of TG but was not in normal glomeruli.
Chronic AMR diagnosis incorporating C4dglom was associated with death-censored allograft failure in TG (P 0.001), regardless of glomerulopathy severity or chronic interstitial fibrosis (P 0.001). C4dglom immunoperoxidase is a promising diagnostic biomarker that has the potential to significantly improve the Banff schema for correctly classifying TG.
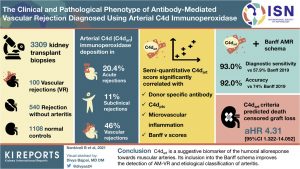 Could endothelial and intimal arterial C4d (C4dart) be a humoral biomarker of endothelial interaction with antibodies in muscular arteria? Would its incorporation into the Banff schema improve the diagnostic sensitivity of antibody-mediated vascular rejection (AM-VR)? These questions were answered by Nankivell and collaborators who, in a recent study, evaluated the clinical utility of C4dart for diagnosis and classification of AM-VR. They compared biopsies with and without arteritis and a negative control group. They found that the addition of C4dart to Banff antibody-mediated rejection increased the sensitivity for AM-VR from 57.9% to 93%, accuracy from 74% to 92%, and specificity from 90.2% to 95.4% versus Banff 2019. The addition of C4dart into the Banff schema improves its diagnostics performance for AM-VR detection.
Could endothelial and intimal arterial C4d (C4dart) be a humoral biomarker of endothelial interaction with antibodies in muscular arteria? Would its incorporation into the Banff schema improve the diagnostic sensitivity of antibody-mediated vascular rejection (AM-VR)? These questions were answered by Nankivell and collaborators who, in a recent study, evaluated the clinical utility of C4dart for diagnosis and classification of AM-VR. They compared biopsies with and without arteritis and a negative control group. They found that the addition of C4dart to Banff antibody-mediated rejection increased the sensitivity for AM-VR from 57.9% to 93%, accuracy from 74% to 92%, and specificity from 90.2% to 95.4% versus Banff 2019. The addition of C4dart into the Banff schema improves its diagnostics performance for AM-VR detection.
This review by Fakhouri et al. discusses the history and future of using and investigating complement inhibitors in kidney diseases. They discuss the roles of complement pathways in different kidney diseases based on a pathogenetic classification.
This classification categorizes the involvement of complement inhibitors into four groups; kidney diseases, which are entirely or mainly driven by complement dysregulation, immune-complex glomerulopathies in which complement activation plays a role, glomerulopathies with non-specific complement-mediated inflammation, and complement-mediated thrombotic microangiopathies.
The authors discuss the choice of potential therapeutic targets within the complement system for different kidney diseases and the current limitations in making these choices. This includes a detailed presentation of the available evidence for using these drugs and current drugs under investigation. Finally, they discuss the complex challenges in treating these rare conditions.
More than ten years after the introduction of eculizumab, and with a growing number of complement inhibitors in development, this article provides a clear summary and rationale on a complex and developing topic.
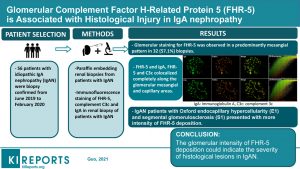 The presence of complement deposition in glomeruli in IgAN suggests that complement may play a role in disease pathogenesis. Factor H–related protein 5 (FHR-5) antagonizes the inhibitory effect of factor H in C3 regulation and leads to over-activation of the alternative pathway. In this study, the authors used immunofluorescence to detect FHR-5 on renal biopsies of 56 patients with IgAN and test plasma for FHR-5 levels using ELISA. They correlated these measures with clinical and pathological markers of disease severity.
The presence of complement deposition in glomeruli in IgAN suggests that complement may play a role in disease pathogenesis. Factor H–related protein 5 (FHR-5) antagonizes the inhibitory effect of factor H in C3 regulation and leads to over-activation of the alternative pathway. In this study, the authors used immunofluorescence to detect FHR-5 on renal biopsies of 56 patients with IgAN and test plasma for FHR-5 levels using ELISA. They correlated these measures with clinical and pathological markers of disease severity.
FHR-5 was observed in a predominantly mesangial pattern in 32 biopsy specimens (57.1%), and it appeared to be co-deposited with IgA and C3c. The authors noted that patients with IgAN and high intensity of FHR-5 deposition in glomeruli showed more severe pathologic manifestations than those with less or without deposition. Circulating FHR-5 levels were elevated in patients with IgAN compared with healthy control subjects and were significantly higher in patients with mesangial hypercellularity at diagnosis than those with nonmesangial hypercellularity. The findings provide more clues to understanding the role of FHR5 in the pathogenesis of IgAN.
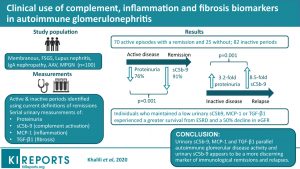 Complement plays a critical role in injury mechanisms of autoimmune glomerulonephritis (GN). One hundred patients with different types of autoimmune glomerulonephritis were included in this prospective cohort study. Proteinuria, urinary sC5b-9, monocyte chemoattractant protein-1 (MCP-1) and transforming growth factor-beta 1 (TGF-b1) ratios were determined using repeated urinary samples collected at follow-ups. Based on current remission definitions for each disease, periods of active and inactive disease were identified.
Complement plays a critical role in injury mechanisms of autoimmune glomerulonephritis (GN). One hundred patients with different types of autoimmune glomerulonephritis were included in this prospective cohort study. Proteinuria, urinary sC5b-9, monocyte chemoattractant protein-1 (MCP-1) and transforming growth factor-beta 1 (TGF-b1) ratios were determined using repeated urinary samples collected at follow-ups. Based on current remission definitions for each disease, periods of active and inactive disease were identified.
Those who did not relapse maintained lower levels of measured biomarkers during inactive periods than those who relapsed. The rise in urinary sC5b-9 was significantly greater than the rise in proteinuria at the time (an 8.5-fold increase compared with 3.2-fold). Urinary sC5b-9 as a complement biomarker appears to be a more discriminating marker of immunologic remissions and relapses, with the potential to parallel disease activity and add clinical value beyond proteinuria.
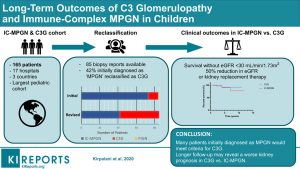 The re-classification of membranoproliferative glomerulonephritis (MPGN) into immune-complex MPGN (IC-MPGN) and C3 glomerulopathy (C3G) has revealed new information about these different diseases. Although adult outcomes in both diseases are poor, pediatric literature is limited to small, single-center cohorts.
The re-classification of membranoproliferative glomerulonephritis (MPGN) into immune-complex MPGN (IC-MPGN) and C3 glomerulopathy (C3G) has revealed new information about these different diseases. Although adult outcomes in both diseases are poor, pediatric literature is limited to small, single-center cohorts.
A retrospective analysis of 165 pediatric patients from 17 hospitals was conducted to compare outcomes between children with IC-MPGN and C3G. Following a review of renal biopsy reports, 42% of patients initially diagnosed with MPGN were reclassified as C3G.
In C3G, steroid treatment was associated with a significant improvement in eGFR compared to no steroids but not in IC-MPGN. This large pediatric IC-MPGN/C3G cohort revealed that nearly half of the patients were misclassified, and C3G may have a worse renal prognosis despite having greater steroid responsiveness. Overall, the prognosis appears to be better than adults; however, persistent hypertension and proteinuria indicate suboptimal disease control.
In this cross-sectional study, Ramachandran et al. performed an internet-based survey among nephrologists in Asia, Africa, and Eastern Europe. The main objective was to assess abilities to perform and interpret a kidney biopsy.
Most respondents were from low-middle-income countries in Africa and Asia. Around two-thirds of respondents reported that biopsies could not be performed in more than 50% of patients suspected of glomerular disease. This proportion was higher in Africa, where half of participants reported that only 10% of their patients could get a biopsy.
Although 75% of nephrologists in the study reported having formal training in performing kidney biopsies and being used to performing them, the absence of a nephropathologist and the high cost meant that kidney biopsies were often not carried out.
Another limitation in diagnosing glomerular disease includes the lack of access to immunofluorescence and electron microscopy. Around 75% of patients covered the cost of diagnosis and treatment themselves. This study highlights the barriers to accessing diagnosis and treatment of glomerular diseases in resource-limited settings.
KIDNEY INTERNATIONAL ARTICLES |
Endothelial-specific Loss of Krüppel-like Factor 4 triggers Complement-mediated Endothelial Injury
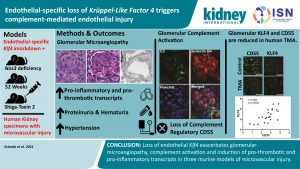 Regardless of the initiating event, kidney thrombotic microangiopathy (TMA) is characterized by complement activation, endothelial cell (EC) gene dysregulation, and microangiopathy.
Regardless of the initiating event, kidney thrombotic microangiopathy (TMA) is characterized by complement activation, endothelial cell (EC) gene dysregulation, and microangiopathy.
Most treatments are supportive, with some subtypes responding to complement inhibition. The loss of EC-specific Krüppel-like Factor 4 (KLF4), an anti-inflammatory and antithrombotic transcription factor, increases susceptibility to TMA and complement activation with a decrease in the complement regulatory gene CD55 in mice model experiments.
Analysis of archived human kidney biopsies with TMA confirmed these findings, with KLF4 and CD55 expression inversely related to the severity of glomerular EC injury. These findings point to a potential role for therapeutics aimed at increasing EC-KLF4 expression.
The Characteristics of Seronegative and Seropositive Non-hepatitis-associated Cryoglobulinemic Glomerulonephritis
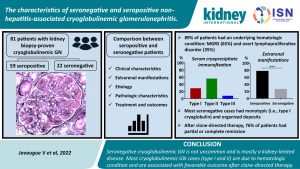 Cryoglobulinemia is often associated with hepatitis infection, but other causes, such as autoimmune diseases, lymphoproliferative disorders, and other infections, have been identified.
Cryoglobulinemia is often associated with hepatitis infection, but other causes, such as autoimmune diseases, lymphoproliferative disorders, and other infections, have been identified.
In this retrospective study performed by Javaugu et al., the authors reported characteristics of 81 patients with biopsy-proven, non-hepatitis cryoglobulinemic glomerulonephritis (CryoGN), including 22 patients with seronegative CryoGN. Three-quarters of patients presented nephrotic syndrome and most of them had an underlying hematologic condition followed by connective tissue disorder.
The main pathologic findings were IgM dominant and polytypic in the seropositive group; half of seronegative cases had monotypic deposits. Deposits were organized in 77% of cases. Acute kidney injury increased the risk of poor kidney outcomes 19-fold. Age was the sole independent predictive factor of mortality.
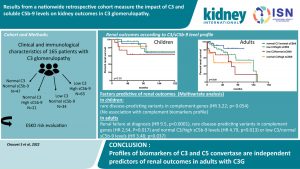
Results From a Nationwide Retrospective Cohort Measure the Impact of C3 and Soluble C5b-9 Levels on Kidney Outcomes in C3 Glomerulopathy
 The prognostic value of complement activation biomarkers in C3 glomerulopathy (C3G) is unknown, and risk stratification remains focused chiefly on non-specific factors such as proteinuria and estimated glomerular filtration rate.
The prognostic value of complement activation biomarkers in C3 glomerulopathy (C3G) is unknown, and risk stratification remains focused chiefly on non-specific factors such as proteinuria and estimated glomerular filtration rate.
Using a retrospective cohort of 165 patients derived from the French National Registry, the authors of this study used multivariate analysis to identify prognosticators of clinical outcomes. Adult onset of disease reduced kidney function, and the presence of rare disease-predicting variants in complement genes predicted the risk of progression to kidney failure.
Additionally, normal C3/high sC5b-9 levels or low C3/normal sC5b-9 levels were independently associated with a worse kidney prognosis, with the relative risk of 3.7 and 8 times higher, respectively.
Subgroup analyses show that these biochemical profiles were associated with more glomerular inflammation, suggesting a mechanistic link. They suggest that more than the degree of convertase activation, the equilibrium between both convertases’ activity – grouped (normal C3/normal sC5b-9 levels or low C3/high sC5b-9 levels) or dissociated (normal C3/high sC5b-9 levels or low C3/normal sC5b-9 levels) – independently correlates with renal outcomes.
The authors propose a three-point C3G prognostic score based on biomarker profiles at risk, estimated glomerular filtration rate at presentation, and genetic findings for risk stratification of patients with C3G and suggest this could be useful in planning management strategies.
Molecular Profiling of Kidney Compartments From Serial Biopsies Differentiate Treatment Responders From Non-responders in Lupus Nephritis
 For clinicians, one of the most challenging and frustrating aspects of managing patients with Lupus nephritis (LN) is differentiating those who will respond to treatment from those who will not. This is mainly because the immune pathways that define treatment response and non-response remain unknown.
For clinicians, one of the most challenging and frustrating aspects of managing patients with Lupus nephritis (LN) is differentiating those who will respond to treatment from those who will not. This is mainly because the immune pathways that define treatment response and non-response remain unknown.
This paper by Parikh et al. goes some way to addressing this paradigm. The authors describe the outcomes of a study looking at kidney transcriptomic analyses in protocol kidney biopsies obtained t flare and after in 58 patients with LN.
Top transcripts were validated, and several identifying markers were established to differentiate clinically complete responders from non-responders. The authors conclude that molecular profiling of kidney biopsies in patients with LN may inform the development of urinary biomarkers which could help clinicians predict treatment responses in these patients.
Complement Activity is Regulated in C3 Glomerulopathy by IgG–factor H Fusion Proteins With and Without Properdin Targeting Domains
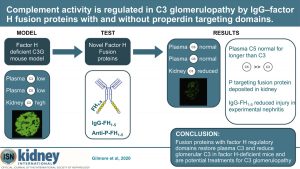 C3 glomerulopathy (C3G) is characterized by abnormal accumulation of complement C3 within glomeruli and glomerular damage due to uncontrolled activation of the alternative complement pathway. One of the causes of this condition is abnormalities in factor H, the major negative regulator of the alternative pathway, specifically its deficiency.
C3 glomerulopathy (C3G) is characterized by abnormal accumulation of complement C3 within glomeruli and glomerular damage due to uncontrolled activation of the alternative complement pathway. One of the causes of this condition is abnormalities in factor H, the major negative regulator of the alternative pathway, specifically its deficiency.
In this study by Gilmore et al., the efficacy of two fusion proteins containing the factor H alternative pathway regulatory domains was assessed. The protein targeted either a non-targeting mouse immunoglobulin (IgG-FH1-5) or an anti-mouse properdin antibody (Anti-P-FH1-5). Both proteins increased plasma C3 and reduced glomerular C3 deposition to an equivalent extent. This study concludes that fusion proteins with Factor H regulatory domains can restore factor C3 in those with factor H deficiency and may be a potential therapy for C3 glomerulopathy.